Home Care Heroes Blog

Managing Post Acute Care Operations in a Storm
How do you manage operations when disaster strikes? Technology and good planning should be your allies.
Storms threaten patient safety and the delivery of post acute care, but a little planning and...
5 Steps for Breaking the Ice with Patients in Therapy & Home Care
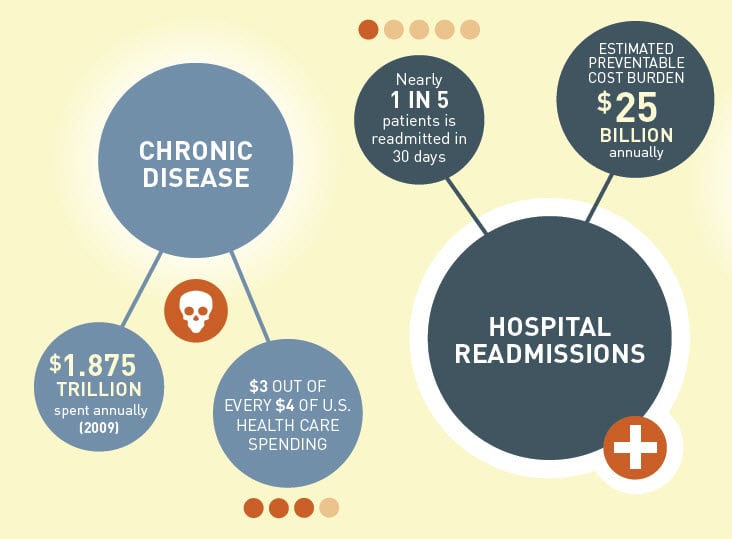
4 Steps for Home Care to Reduce Readmissions
5 Things No One Told Me Before I Launched an ACO
"If I had known then what I know now..."
CMS Penalties for Avoidable Readmissions Have Started
The entire healthcare world has known for a long time that yesterday was coming: the day that CMS started penalizing hospitals for what are called avoidable readmissions. That's right--THAT just...
Population Health IT for ACOs
Stay Informed with our Podcast!
Need Help


Simplify care delivery. Improve outcomes. Start with Ankota.
Trusted by home care agencies nationwide